Presentation:
Since Sarah’s initial episode of severe low back pain 9 years previously she had made a remarkable recovery. She was able to play her beloved basketball and happily engage in her other favourite thing, gardening.
While she had experienced occasional relapses over that time, they were nothing like the first episode and always resolved completely with timely adjustments. She was an excellent patient; always following instructions and advice, and staying regular with her maintenance.
Symptoms:
On 9th October 2014 Sarah had tipped over a heavy concrete birth bath so she could clean it. As she tried to lift it upright again, she felt a sudden shot of severe pain across her lumbosacral junction. This was soon accompanied by muscle spasm and antalgia. She could walk but with difficulty and required assistance.
She was helped inside and onto her bed where the only comfortable position for her was supine with her two pillows under her knees. She was given an ice pack which was applied in a cycle of 20min on, 20min off, repeated for 2 hours, a break for 2 hours and repeated again.
The combination of rest and ice reduced the pain enough for her to have a night of broken sleep. The following day she reported that the low back pain was slightly better but she now had full right leg sciatica and a strongly positive Valsalva sign. There was no indication of Cauda Equina.
Examination:
Sarah was able to get to the clinic the following day but was clearly in a lot of pain. She was antalgic to the right and the paraspinal muscles were effectively rigid.
Orthopaedic:
Lumbar ranges of motion were all but impossible to test due to the muscle spasm. Any attempt to put her through them would have been both futile and possibly hazardous.
Due to the Hi-Lo action of our treatment tables we were able to gently lower her into a prone position where an examination could better performed.
Prone leg length comparison showed a slight shortening of the right leg. She could tolerate a unilateral Nachlas test on either side, but only to ~40° before pain started. A bilateral Nachlas test was not possible beyond ~20°. Anything involving pelvic nutation was painful. It was not possible to test her Gluteal or Hamstring strength due to the level of pain.
Neurological Examination:
The Right Patella and Achilles deep tendon reflexes were markedly reduced (1/5)
Sarah reported no numbness or paraesthesia, however she was unable to heel walk easily on the right.
Imaging:
On the basis of the above test results, it was clear that Sarah had suffered a significant disc injury, most likely at L5-S1. It was determined that she needed an MRI to evaluate the extent of the injury, so she was referred to Victoria House Medical Imaging for a 3T MRI (see images and report below)
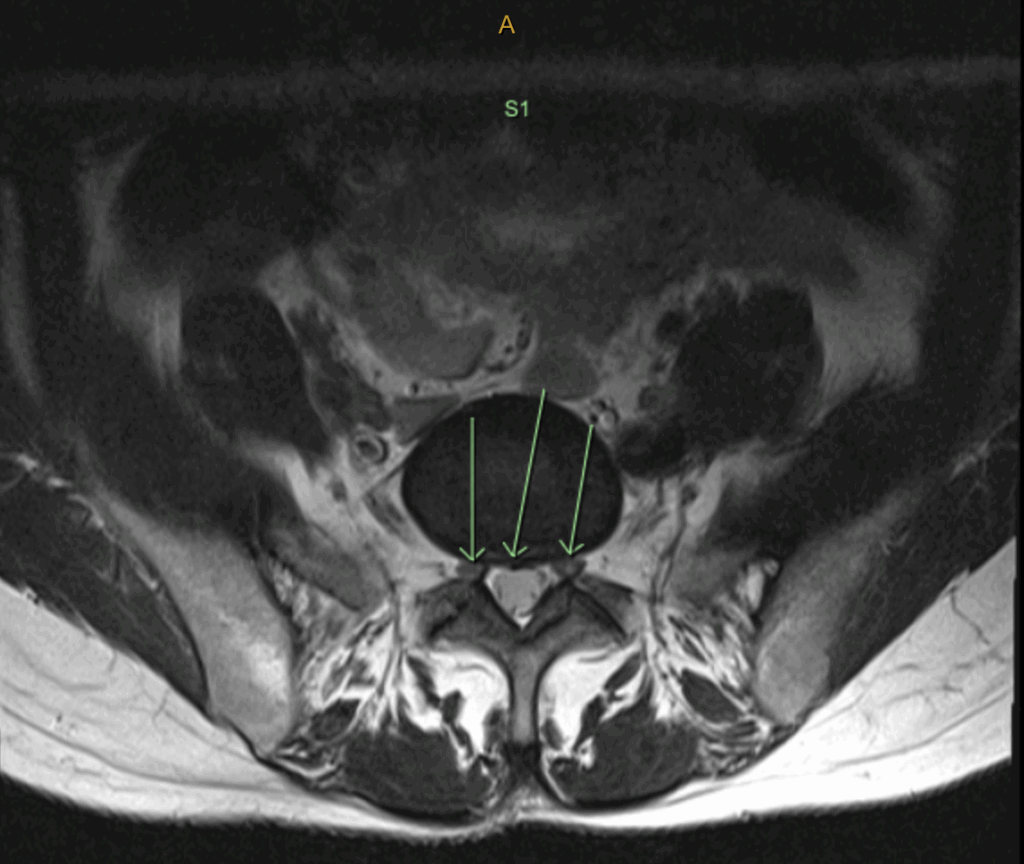
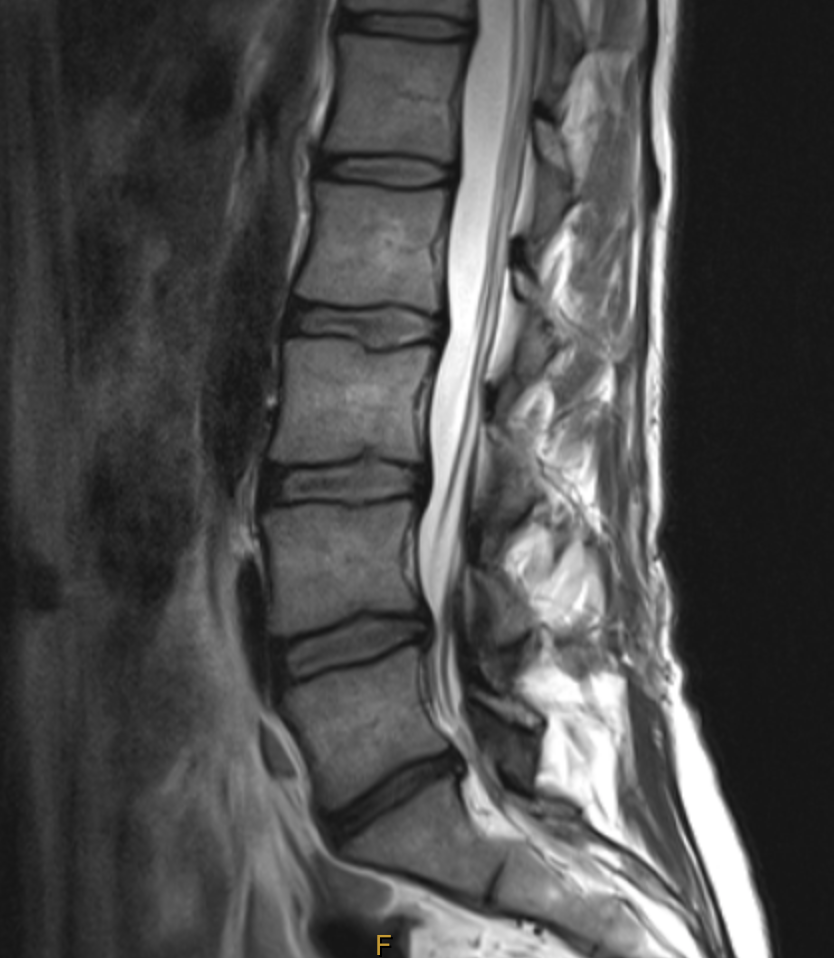
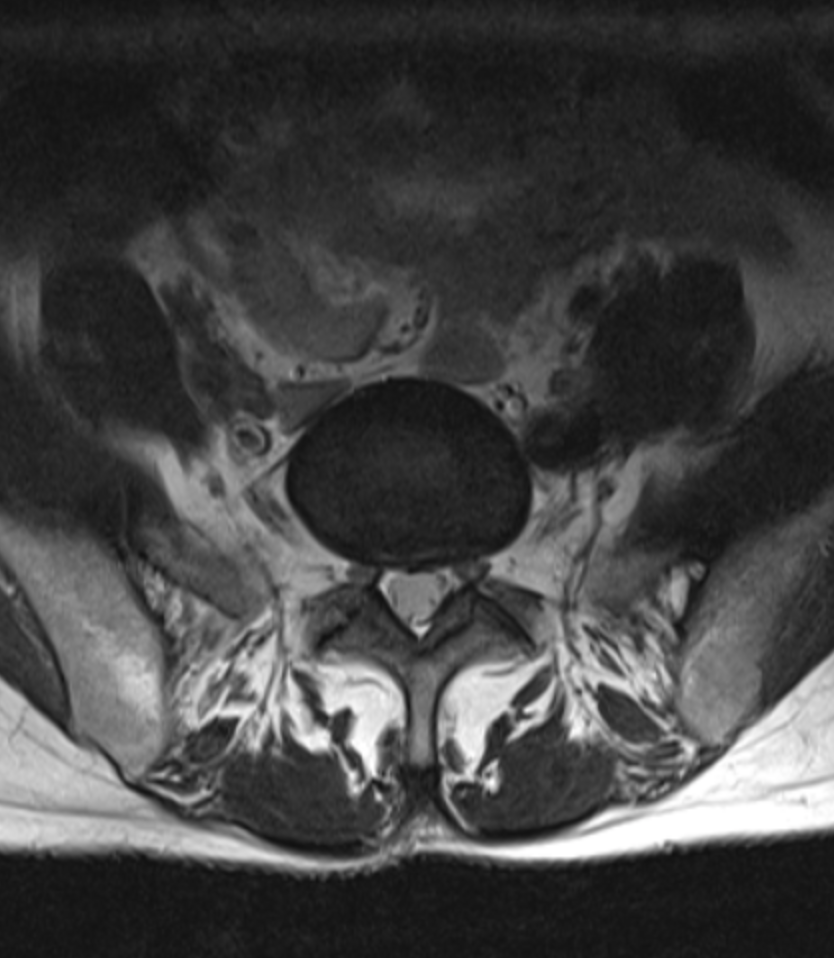

Diagnosis:
The images confirmed the diagnosis – this was indeed a significant disc injury.
The quality and accuracy of this Radiology report are orders of magnitude above her previous report. This shows the importance of choosing your Radiology providers carefully and building a good relationship with them. If they know you’re going to read the films and not just the report, they’ll go to extra effort to show you what’s going on.
If you send them a sloppy referral they won’t go to any more effort than necessary.
If you call them and ask them to clarify or explain something you don’t understand, you’ll almost always find that they’re extremely willing and helpful. Like everyone, they love to know that their work is appreciated.
The green arrows are pointing out the annular fissure that’s an early feature of disc injury. The injury starts off as a series of small, concentric fissures. With time and further stresses the intradiscal pressure forces the nuclear material through each fissure, like lava ascending the Earth’s crust on it’s way to forming a volcano.
Report of Findings:
When Sarah presented for the Report of Findings the following day we went through the films and test results together.
I explained to her that this had probably been coming for a long time.
The previous films showed narrowing of the L5-S1 disc, so we know there had been at least one injury prior to the 2013 episode that was either asymptomatic or so mild that it was passed off as something inconsequential.
The previous episode 9 years ago was almost certainly the first substantial injury to the disc, and had left an area of damage that predisposed her to future issues.
Up to a point, each injury usually becomes asymptomatic eventually, but the damage always remains. This is because the disc has a very poor blood supply*2 so it only ever repairs with scar tissue, not disc material.
The intradiscal pressure is so high that the heart can’t push blood against it, so the disc “steals” it’s nutrients from it’s neighbours through osmosis. Waste material is “squeezed” out through the pumping action of day-to-day movement. That’s one of the reasons why sedentary people tend to have a greater likelihood of disc injury *1.
One of most poorly understood features of the disc by patients (and some Drs) is that the nerve supply only extends ~1/3 of the way into the disc substance *2. Two reasons for this are:
- The pressure inside the disc is too high for the nerves to survive.
- The nuclear material is neurotoxic.
Tears within the disc tend to propagate from the inside toward the outside: the softest structures tear first. Due to the fact that the nerves only penetrate ~1/3 of the into the disc, you need to tear it ~2/3 before you feel anything. Even then, it’s only a dull ache and often dismissed as a “pulled muscle” or “strained back”.
It was also pointed out that, in light of the fact that both parents had suffered from similar injuries, she had almost certainly inherited this tendency.
Although the injury at L5-S1 was the current problem and could be managed, of greater concern now was the risk of an even worse injury happening at L4-L5 in the future. I therefore had to give her the unwelcome news that her basketball career was probably over.
During the Report of Findings I told her that if she were to injure this area again, it could be much worse than anything she had experienced to date. This is where the issue of Adjacent Segment Disease (ASD) *3 comes into the picture. Whenever a motor unit loses it’s movement, that motion and it’s associated loads are passed on to the unit above. The excess loads accelerate wear in the newly loaded segment, thereby passing the problem up the chain.
This is why surgical fusion has fallen out of favour except in the most extreme cases of instability. However, one can still have a state of effective fusion through loss of disc height & elasticity as a result of injury.
The L5-S1 disc was narrowed when we first we saw Sarah, and now it was damaged again, more severely. At that time she already had some bulging of the L4-L5 disc and was therefore now a prime candidate for ASD *3 .
Treatment Given:
Over the following 3-4days, Sarah’s pain gradually subsided to the point where I could adjust her.
Testing confirmed that the system most likely to help her was AMCT, so we began adjustments twice per week. I used the AMCT analysis protocol using an Impulse iQ instrument.
The most common listings were Right Medial Meniscus, Left AS, Right PI, Right L5, Right L3, Right T12, Right T7 and Right C5. The iQ was set at Level 1 for the Medial Meniscus and C5, Level 3 for Pelvis and Lumbars, and Level 2 for the Thoracics.
Progress & Outcome:
Sarah’s progress was gradual. She had several episodes of relapse; sometimes triggered by a particular action or position, other times they were inexplicable.
After a period of approximately 8 weeks her symptoms had reduced to the point where she could go about her daily activities with caution. Any periods of prolonged sitting (more than 45min-60min), would cause her spine to go into protective muscle contraction. This was not a sudden spasm but gradual contraction that would render the area totally immobile. Gentle walking would usually release the contraction within 10min-15min.
By 6 months Sarah was able to do everything in her usual fashion provided she did it mindfully.
Links & Further Information
1 – Disc Injury in the Sedentary
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4152382
2 – Disc Innervation and Blood Supply
https://www.ncbi.nlm.nih.gov/books/NBK470583
3 – Adjacent Segment Disease (Adjacent Joint Disease)
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3963057
https://pubmed.ncbi.nlm.nih.gov/25102498
“If it’s never been right, you don’t know it’s not right until it hurts.
Once it’s been right, you’ll know as soon as it’s not before it hurts.”

