Sarah – The Grand Final
It’s time for full disclosure. The “Sarah Case” is actually the “Joely Case”.
When we started these cases we thought it best to protect her privacy. But then as I was writing this final chapter, we both decided to let everyone know that it was actually Joely. One of the reasons she has so much empathy for patients who’ve suffered catastrophic injuries is that she has been through it.
Saturday
It was AFL Grand Final Day, 30th September 2017.
In time-on of the third quarter, Dusty Martin took possession 25m out and fed the ball out to Jason Castagna, who snapped over his shoulder to effectively put the game beyond the reach of Adelaide, who trailed by 34 points at three quarter time.
Joely was a Tigers Tragic. In her excitement at Dusty’s winning play, she leapt to her feet from the low couch and cheered. Her excited cheering was stopped in an instant when she felt a searing pain shoot across her lower back and down over her left buttock.
She went into the early stages of shock with pallor, sweating and nausea. We tried to walk it off by gingerly walking 20m-30m but it made no difference. She took 2 Nurofen and 2 Panadol Osteo in an effort to control the pain.
The 42km drive home was made with Joely lying as flat as possible with the car seat laid back as far as it would go. Although she was relatively comfortable in this position, she was still hit with occasional stabs of severe pain.
We called our friends at Victoria House Medical Imaging and booked her in for an emergency MRI the following day at 9:00am.
Late that night it became clear that she was going to need more than over-the-counter pain relief, so we went to the local Private Emergency hospital. She was given Endone and an unspecified intramuscular anti-inflammatory. At around 3:00am the following morning she roused from broken sleep and told me that her left leg was now numb from the top of her pelvis to just above the knee.
Sunday
By the time we’d driven the 1hr to VicHouse the following day, she could stand with difficulty but needed help to walk. The numbness has extended to the sole of her foot. She could not undress herself.
I sat in the control booth with the MRI Radiographer while the scan was done and could see the life changing images reveal themselves as the scan progressed. There was total central posterior disc extrusion at L4/5 with severe spinal canal stenosis. Displacement and compression of the nerves of the Cauda Equina were the icing on the cake.
As we drove home I received a call from Dr Frank Malara, one of the senior Radiologists at VicHouse confirming the diagnosis.
(see images below)
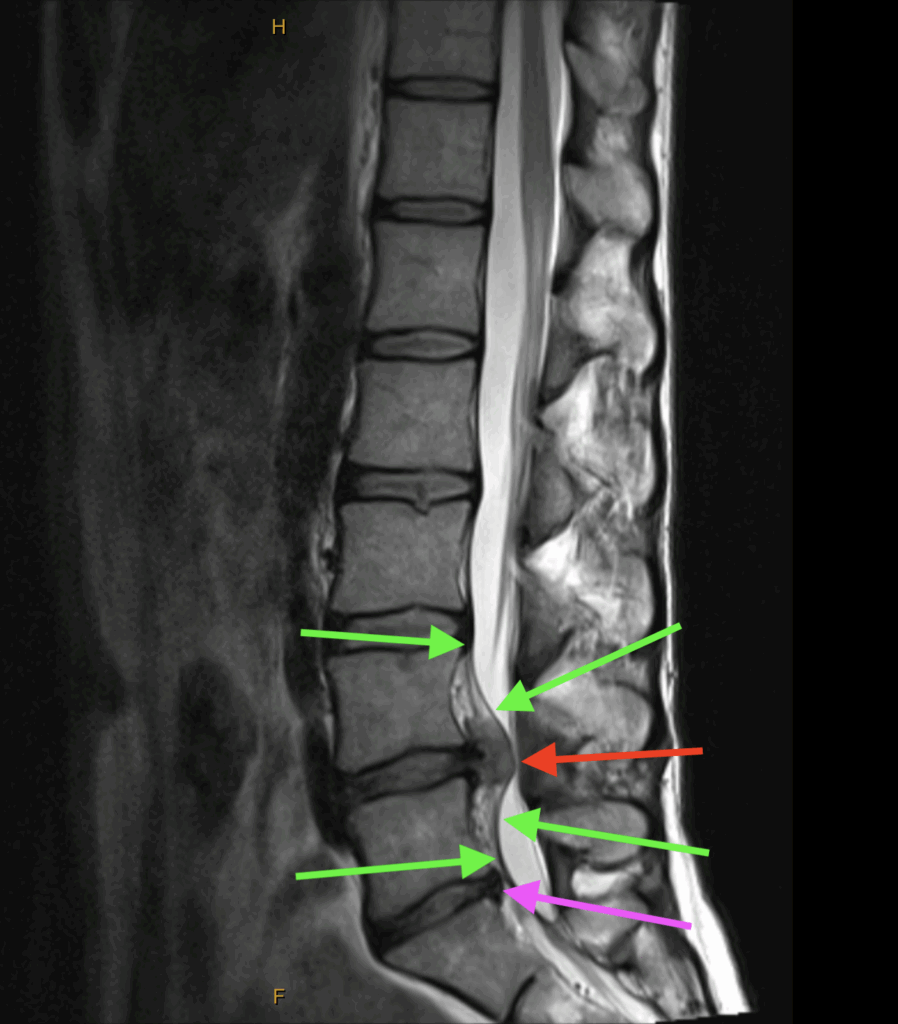
T2 Sagittal
The green arrows indicate the Posterior Longitudinal Ligament. Note how it’s been torn off the anterior wall of the central canal by the extruded disc material. The mottled appearance between the ligament and the anterior wall is blood and torn tissue.
The red arrow indicates the mass of extruded nuclear material.
The purple arrow indicates the desiccated remnants of the previous L5-S1 disc.
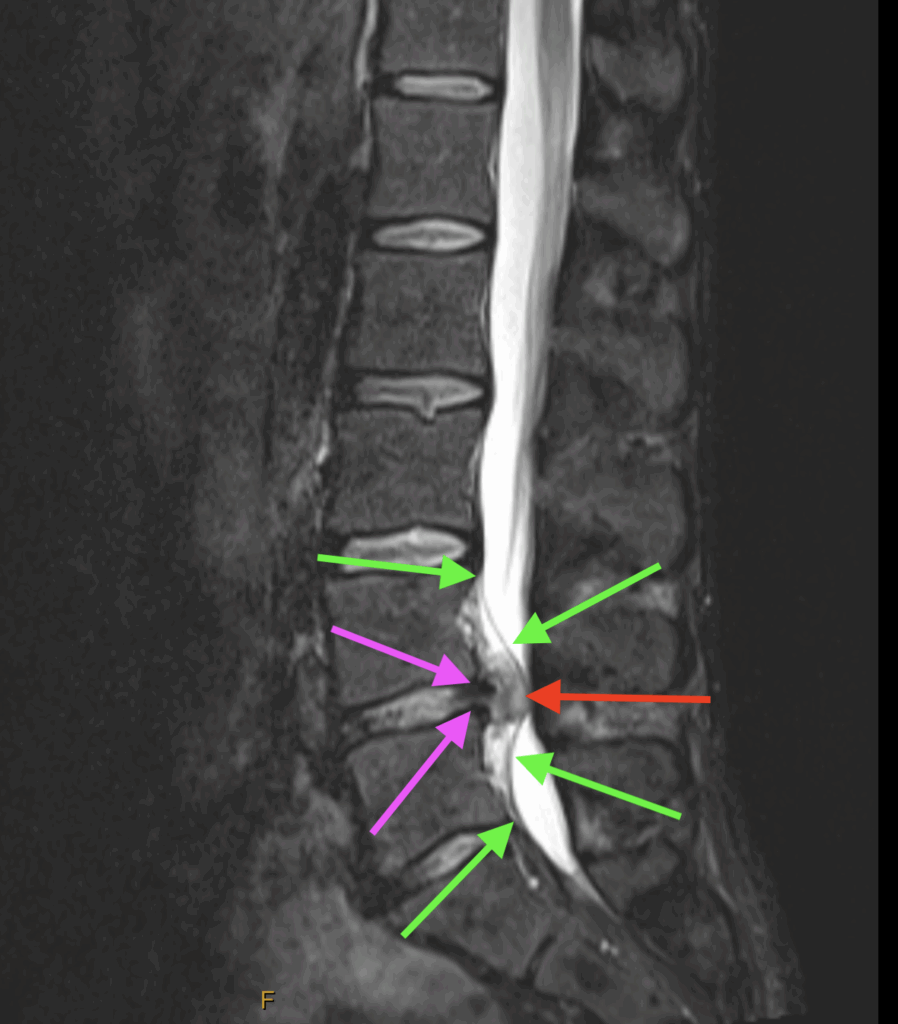
STIR Sagittal
The purple arrows indicate where the posterior margin of the disc is torn open.
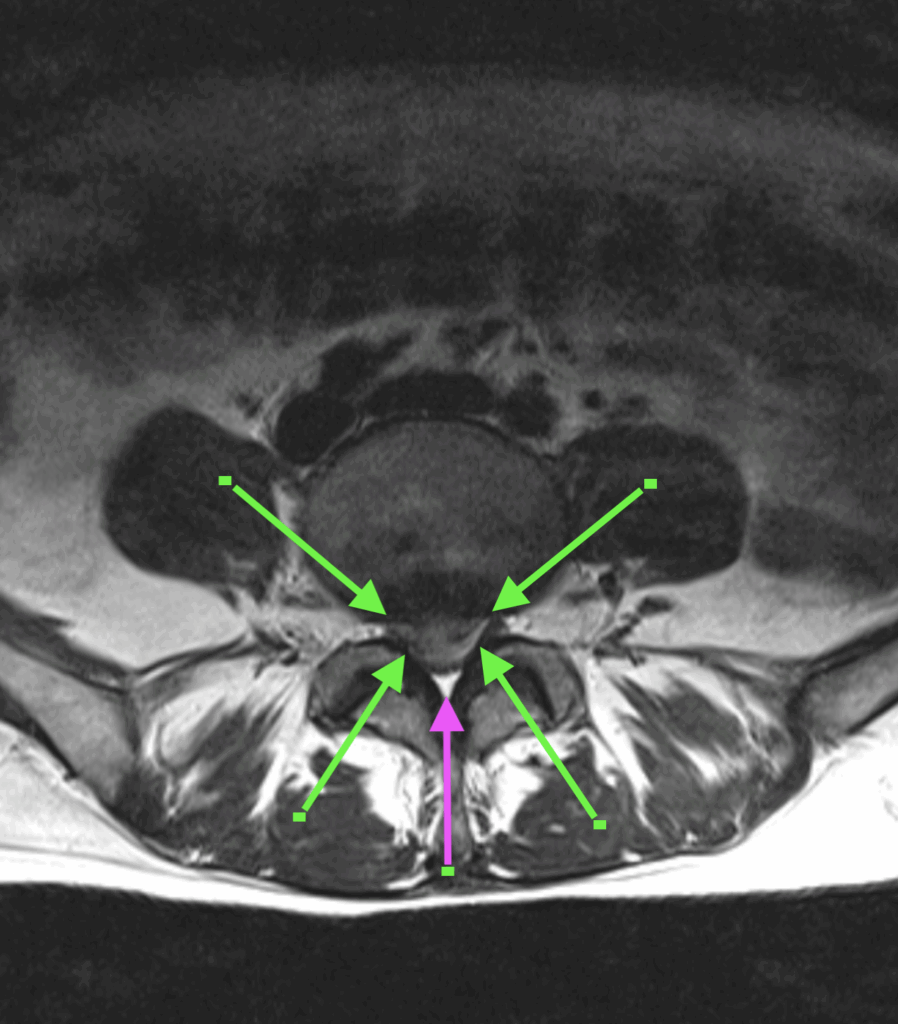
T2 Axial
The green arrows indicate the margins of the extruded disc material. Between the tips of each arrow we can see where the nerves of the Cauda Equina have been forced apart and into the lateral recess.
The purple arrow indicates the remaining space in the central canal.

There was no question that Joely needed spinal decompression surgery as soon as possible.
One the way home we called a local GP near where we lived and asked for the first available appointment. When we got there we told the GP what had happened and said that Joely needed a referral for a microdiscectomy, stronger pain relief and muscle relaxants.
The GP was very reluctant, so I showed him the MRI to which he responded “I can’t read those”. So I pointed out the disc injury.
He then said that “We don’t normally suggest surgery for back pain. We normally prescribe anti-inflammatories and six weeks of rest and Physiotherapy.” At this stage patience was running thin but I summoned all my calmness and said that without surgery she will mostly likely suffer permanent paralysis at best. He very reluctantly wrote the referral and gave Joely a prescription for Endone and Valium.
Monday
We had a very difficult night with only fleeting periods of sleep. By the morning Joely had started to develop foot drop.
We called our dear friend and Orthopædic Surgeon Dr David de la Harpe as soon as his rooms were open and asked for the first available appointment, which was at 9:00am on Tuesday.
Tuesday
By the time we saw David he’d already seen the MRI images online. There was no need for any further examination. David said that he’d admit Joely to a ward immediately but he needed his “A-Team” to help him with this case, which would mean waiting until Thursday before the surgery could be performed.
He also explained that there was so much tension on the dura that there was a high risk of it splitting lengthwise if it was disturbed. He went on to say that when that happens the nerves of the Cauda Equina spill out into the canal like cooked spaghetti, the CSF runs out of the longitudinal split and patient dies on the table. That meant that he and his Assistant Surgeon had to coordinate both the timing and degree of their excisions so the dura was not pulled one way or the other as the tension was relieved.
Wednesday
Joely’s leg was now effectively flaccid, she had lost both the anterior and posterior tibial pulses and her lower leg was starting to change colour.
Thursday
Joely was first on the list, and returned to the ward after two and a half hours of surgery.
David came into the room and told us that surgery was “extremely challenging but successful” and now it was up to Joely’s body to do the rest.
We’ll cover the result of the surgery and final outcome in the Discussion…

