Presentation:
Jane, a 64 year old lady called the clinic asking for an appointment. She’d been referred to us by her son and daughter-in-law. He had previously undergone unsuccessful management of severe lumbo-sacral pain, knee and hip pain. Jane passed the First stage of our Three Stage Filter – she was referred by another patient.
Symptoms:
Jane’s chief complaint was a one month history of sudden onset Right sciatica extending from her buttock to the sole of her foot. Nothing seemed to make the pain either better or worse – it was constant and unrelenting. There was no Valsalva sign and no indication of Cauda Equina Syndrome. Seems pretty innocuous so far.
She had been diagnosed as having a “sciatic nerve problem” and treated by an Osteopath. She was treated with Soft Tissue Therapy and manipulation.
Jane was also suffering from Right anterior knee pain. This had been present for approximately 6 months, was of sudden onset, unknown etiology, worsened by descending stairs and relieved by elevating her leg.
She had been diagnosed as having a “slipped patella” and treated by the Osteopath without success. This was also treated with Soft Tissue Therapy and manipulation.
History:
While Jane had not suffered any previous major falls, fractures, dislocations, car accidents or loss of consciousness, she did have an extensive medical and surgical history.
She had undergone:
- Tonsillectomy at 8yo
- Vaginal cyst removal, D&C and tubal ligation in 1994
- Cholecystectomy in 2001
- Abdominoplasty in 2003
- CSF leak repair following surgery for a Sphenoid Meningeoencephalocele in 2007
- Insertion of a pressure monitor for the Sphenoid Meningeoencephalocele later in 2007
- Hiatus Hernia repair in 2008
- Left Post Facial Craniotomy and MVD (Janetta procedure) of the Trigeminal nerve in 2012
- Surgical decompression and fusion of L4/5 in 2014
She was taking:
- Lyrica 150mg morning and night
- Coversil Plus 1.25mg+4mg
Examination:
Jane was quite short in stature and in her own words, “a little overweight”.
Orthopaedic:
Cervical ranges of motion were:
- Flexion – 50° – no pain
- Extension – 40°- no pain
- Left Rotation – 60°- no pain
- Right Rotation – 60°- no pain
- Left Lateral Flexion – 20°- no pain
- Right Lateral Flexion – 20°- no pain
This is not an unusual finding in a patient of this age and this endomorphic body type.
Lumbar ranges of motion were:
- Flexion – 60° – no pain
- Extension – 10°- no pain
- Left Rotation – 10°- no pain
- Right Rotation – 10°- no pain
- Left Lateral Flexion – 10°- no pain
- Right Lateral Flexion – 10°- no pain
Once again, not unusual for the same reasons as above. Add the hard fusion of L4-5 to the mix and there’s not going to be a lot of free motion available.
SLR was normal on the Left, but produced some pain and pulling into the gluteals at 40° on the Right. This is a bit more interesting. Possibly indicative of dural traction from the fused area, but more likely from SIJ dysfunction.
Patrick FABER was strongly positive bilaterally with localised deep pain around the posterior greater trochanters.
After her Initial Consultation and Examination I went through her Radiographic history back to 2003. One of the relevant findings was that she had been diagnosed with “mild osteoarthrosis” in both hips. Unlike fine wine and violins, arthritis does not improve with age. Having said that, one must be careful not to attribute current symptoms to old findings on the basis of assumption. Correlation does not equal causation.
Supported Adams, Cervical Compression and Maigne’s were all normal.
Examination of the right knee revealed increased lateral mobility across the tibial plateau and palpable-audible fine crepitus behind the patella on active flexion/extension.
The increase in lateral mobility across the tibial plateau points to either laxity of the collateral ligaments or both, whereby reduced joint space due to the arthritic degeneration creates relative laxity of the collateral ligaments. Jane mentioned after the exam that she hurt her knee quite badly water skiing several decades ago.
The crepitus under the patella on seated flexion and extension is a very clear indicator of Chondromalacia Patellae. This simple test can save you time, and save the patient from having unnecessary films.
Neurological:
All tendon reflexes were 2+
All cervical myotomes were 5+
All lumbo-sacral myotomes were 5+ except Right Hamstring, Glute Max & Gastrocnemius – 4+ Now we’re starting think L4-5-S1 involvement.
Images provided by the patient:
17/12/2013
We can see anterolisthesis of L4 on L5, most likely due to facet arthrosis
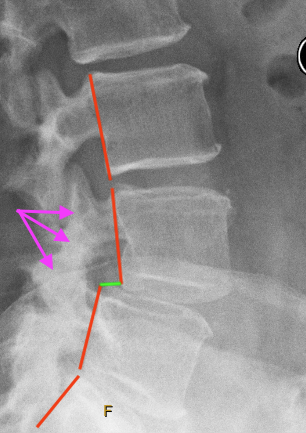
A better view of the anterolisthesis and arthrosis
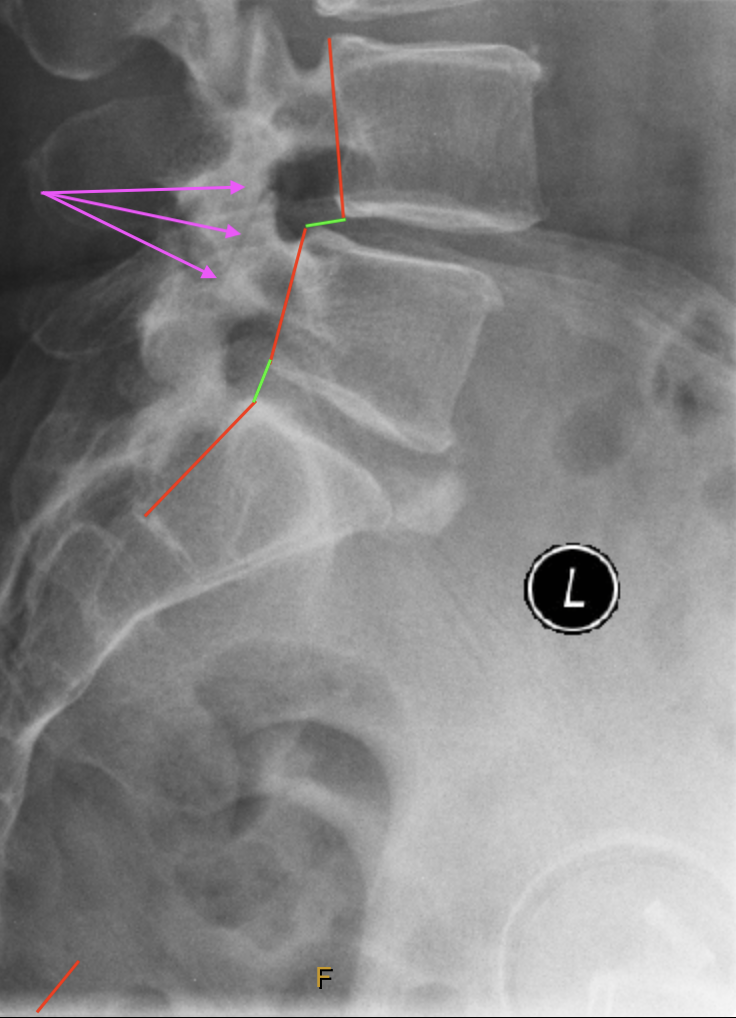
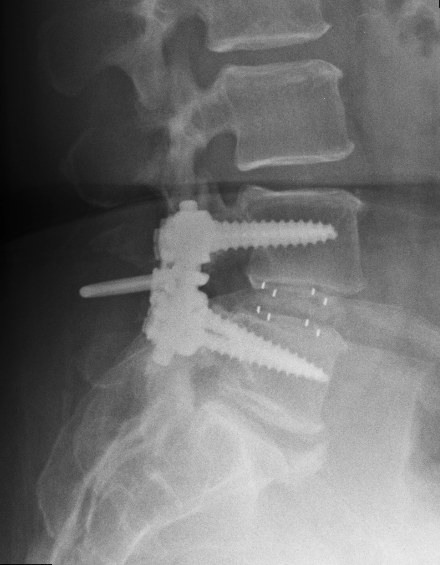
24/04/2014
This is post surgery showing the pedicular screws, rods, transverse bar and inter-transverse process bone graft chips. Incidentally apparent (but not reported) is the sclerosis on the iliac side indicating sacaroiliitis on the left.
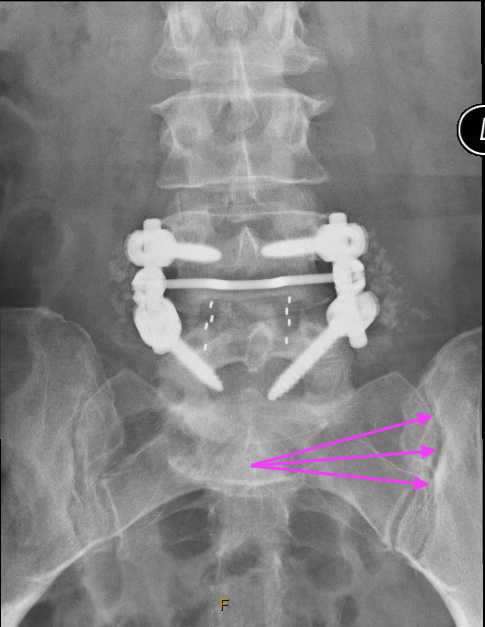
What Is Your Provisional Diagnosis?
Right sacroiliac dysfunction.
Post traumatic knee dysfunction leading to maltracking induced Chondromalacia Patellae and laxity of both the medial and lateral collateral ligaments.
If You Have A Differential Diagnosis or Diagnoses, What Is It (or They)?
Piriformis Syndrome – unlikely considering the pain extends the full length of the leg.
Adjacent Joint Disease causing disc/neural irritation at the segment above – unlikely due to the pain distribution pattern.
What Further Tests (if any) Would You Do?
The Piera-Wenban Test – this indicated that although the films from 2014 showed sacroiliitis on the left, the true problem was SIJ dysfunction on the right. It also showed that while AMCT would probably help, SOT was the technique of choice. It further indicated that Jane was a Category 3 on the right.
Is This A Chiropractic Case?
Yes.
Jane has passed the Second Stage of our Three Stage Filter – I’m sure I can help her to a large extent.
Jane was a delight. Despite the horrors that she had endured previously, the surgery and the failed treatment, she was confident and positive. She passed the Third and final stage of our Three Stage Filter.
Diagnosis and Treatment
After Jane’s Initial Consultation and Examination we made another appointment for the following week. With her express permission, this gave me time to go through all of her previous tests results and images.
This level of access is one of the major benefits of building close working relationships with your patient’s other health professionals. In Jane’s case we had access to all of her imaging, plus her full medical history.
During the report I explained to Jane that the site of the surgery was not the cause of her pain and that I would not be manipulating that area. That was an enormous relief to her because she was justifiably nervous about having that area disturbed.
I explained what and where the true issue was and how we would be managing it. She was very happy to get started, so we adjusted her that day with the following listing:
Category 3 Right, Neutralise T5 CMRT (Activator 2 set at 2 rings)
Left C5 (Activator 3 set at three rings, through my finger)
Right C3 (Activator 3 set at three rings, through my finger)
Next appointment in 3 days.
At her next appointment Jane reported that the sciatica had reduced from 8/10 to 4/10, her neck had a better range of motion and she had been sleeping much better.
She was tested again using the PW Test which confirmed that she had responded very well. There a much lower lag-time in her responses at all levels.
Her listing that day was again:
Category 3 Right, Neutralise T5 CMRT (Activator 2 set at 2 rings)
Left C5 (Activator 3 set at three rings, through my finger)
Right C3 (Activator 3 set at three rings, through my finger)
This time I was able to adjust her knee as well. This was all done with an Impulse iQ using the following listings based on AMCT protocol:
Right anterior proximal tibia
Right external proximal tibia
Right posterior proximal fibula
Right inferior patella.
The iQ was set at Level 2 and allowed to run through it’s cycle to completion.
Given her positive response we decided to continue assessment and treatment twice per week until testing indicated that she was holding her adjustments. Experience had shown that it would probably take somewhere between 2 weeks for symptoms to respond and 4-6 months for stabilisation, so we would be guided by the testing at each visit.
Progress
Over the following three weeks, Jane’s sciatica gradually reduced to ~1-2/10. The knee pain had disappeared completely and, while the crepitus was still palpable, it was markedly reduced. By the fourth week she had only very slight bilateral hip pain at the extremes of the Patrick FABER test.
Her listing remained the same throughout her time with us with the exception of one appointment where she had missed the last step at the bottom of the staircase. She jarred her lower back and knee quite severely and was in a lot of discomfort. In that case The PW Test indicated AMCT, Left AS major.
Her listing was:
Left AS, Left T12, Left C5
All were performed using AMCT contacts with the Impulse iQ set to Level 3 for the pelvis, Level 2 for the Thoracics and Level 1 for the Cervicals. In each case the Instrument was allowed to run through it’s full cycle.
At the following appointment she was symptom free. Testing confirmed that the original adjustment sequence was once again appropriate.
Jane transitioned smoothly through being seen twice per week, to weekly, to ten-day intervals, fortnightly and then on to monthly maintenance over a period of 18 weeks. She was still holding her adjustments with monthly maintenance when I retired.
Every decision point for the reduction of her treatment was test-based, not formula-based.
Discussion
One reason for including Jane’s case is that she was a prime example of the Headline Ailment Syndrome. This is where the patient has a history of, or current activity of a major problem. These problems are usually spectacular; such as malignancy, neurodegenerative disorders, autoimmune diseases etc.
The presence of these problems can distract the Clinician from the true cause of the issue at hand. We have seen many cases where the patient has been diagnosed with something like cancer for example. From the time of that diagnosis, every symptom the patient ever reports is blamed on the Headline Ailment. The travesty spawned at that point is that the patient is only ever managed for the Headline Ailment – almost as if you’re only allowed to have one problem at a time.
All patients are entitled to more than one problem. In fact, they are more likely to have comorbidities when there’s a Headline Ailment in progress.
In Jane’s case she had a host of spectacular and clinically interesting problems, none of which had anything to do with her sciatica and knee pain.
The other reason for including Jane’s case is to illustrate the importance of having a variety of techniques in your repertoire. Not all patients fit one technique system, so if you only know one system you need to make everyone fit what you know, rather than adapting the treatment to fit the patient. Furthermore, it’s a good idea to have a range of technique systems that are compatible e.g. AMCT-SOT-NMI or Gonstead-Diversified-Thompson etc.
The greater your range of technique proficiencies, the greater the range of patients you can help. But make sure you ARE proficient; don’t become a Jack-of-All-Trades but Master-of-None.
Finally, make sure you have reliable and repeatable before-and-after tests that demonstrate to both the patients and you that you are doing the right thing.
In Closing
This has been an extremely interesting year for us. At first we were shocked by the sense of disillusionment and abandonment that the newest members of our most beautiful profession had been experiencing. Then we were saddened by the number of our more senior members that were suffering from burnout and thinking of leaving the profession.
After listening to over 300 of you gorgeous Doctors share your stories, your fears and your victories, we came away truly awed by your bravery, your dedication, your love of our profession and your willingness to support each other.
We are now certain that while ever we keep looking after each other, everyone is going to be just fine. We will all move our profession forward with courage, integrity and love.
Joely and I wish you all a beautiful Christmas filled with laughter and joy, and a New Year filled with success, health and happiness.
Love to All,
Dr Rob & Joely


