Sarah – The Grand Final
It’s time for full disclosure. The “Sarah Case” is actually the “Joely Case”.
When we started these cases we thought it best to protect her privacy. But then as I was writing this final chapter, we both decided to let everyone know that it was actually Joely. One of the reasons she has so much empathy for patients who’ve suffered catastrophic injuries is that she has been through it.
Saturday
It was AFL Grand Final Day, 30th September 2017.
In time-on of the third quarter, Dusty Martin took possession 25m out and fed the ball out to Jason Castagna, who snapped over his shoulder to effectively put the game beyond the reach of Adelaide, who trailed by 34 points at three quarter time.
Joely was a Tigers Tragic. In her excitement at Dusty’s winning play, she leapt to her feet from the low couch and cheered. Her excited cheering was stopped in an instant when she felt a searing pain shoot across her lower back and down over her left buttock.
The lumbar lordosis decreases when we sit. This reverses the disc space shape from wedged toward the front, to wedged toward the back which tends to push the nuclear material towards the back of the disc. Joely’s previous series of disc injuries created multiple annular fissures which weakened the structural integrity of disc.
She was sitting on a very low couch, which meant that her knees were higher than her hips, reversing the lordosis and putting even more stress on the discs. The explosive effort of jumping up from this position, in conjunction with the spiking intra-abdominal pressure from the scream of excitement created massive intra-disc pressure – the “Valsalva Manoeuvre from Hell”.
The nuclear contents ripped through the already compromised and fissured annulus with such force that when it shot out of the posterior margin of the disc it slammed the Cauda Equina into the posterior wall of the central canal with enough force to bruise the wall.
She went into the early stages of shock with pallor, sweating and nausea.
The body instantly recognises when there’s a severe injury and immediately tries to minimise further damage.
We tried to walk it off by gingerly walking 20m-30m but it made no difference. She took 2 Nurofen and 2 Panadol Osteo in an effort to control the pain.
This was a case of knowing it was bad but hoping it wasn’t.
The 42km drive home was made with Joely lying as flat as possible with the car seat laid back as far as it would go. Although she was relatively comfortable in this position, she was still hit with occasional stabs of severe pain.
We called our friends at Victoria House Medical Imaging and booked her in for an emergency MRI the following day at 9:00am.
There was never a question about imaging. It was not a matter of “Is it bad?”, it was more a case of “It’s really bad, but is it catastrophic?”
Late that night it became clear that she was going to need more than over-the-counter pain relief, so we went to the local Private Emergency hospital. She was given Endone and an unspecified intramuscular anti-inflammatory. At around 3:00am the following morning she roused from broken sleep and told me that her left leg was now numb from the top of her pelvis to just above the knee.
If you ever come across a case of rapidly peripheralising symptoms such as this, consider your next move very carefully. Your patient is in imminent peril.
Sunday
By the time we’d driven the 1hr to VicHouse the following day, she could stand with difficulty but needed help to walk. The numbness has extended to the sole of her foot. She could not undress herself.
I sat in the control booth with the MRI Radiographer while the scan was done and could see the life changing images reveal themselves as the scan progressed. There was total central posterior disc extrusion at L4/5 with severe spinal canal stenosis. Displacement and compression of the nerves of the Cauda Equina were the icing on the cake.
As we drove home I received a call from Dr Frank Malara, one of the senior Radiologists at VicHouse confirming the diagnosis.
This further illustrates what we’ve said previously about building good relationships with other professionals. Without that relationship we would have been in the Public System totally at the mercy of whoever happens to be rostered on that day.
(see images below)
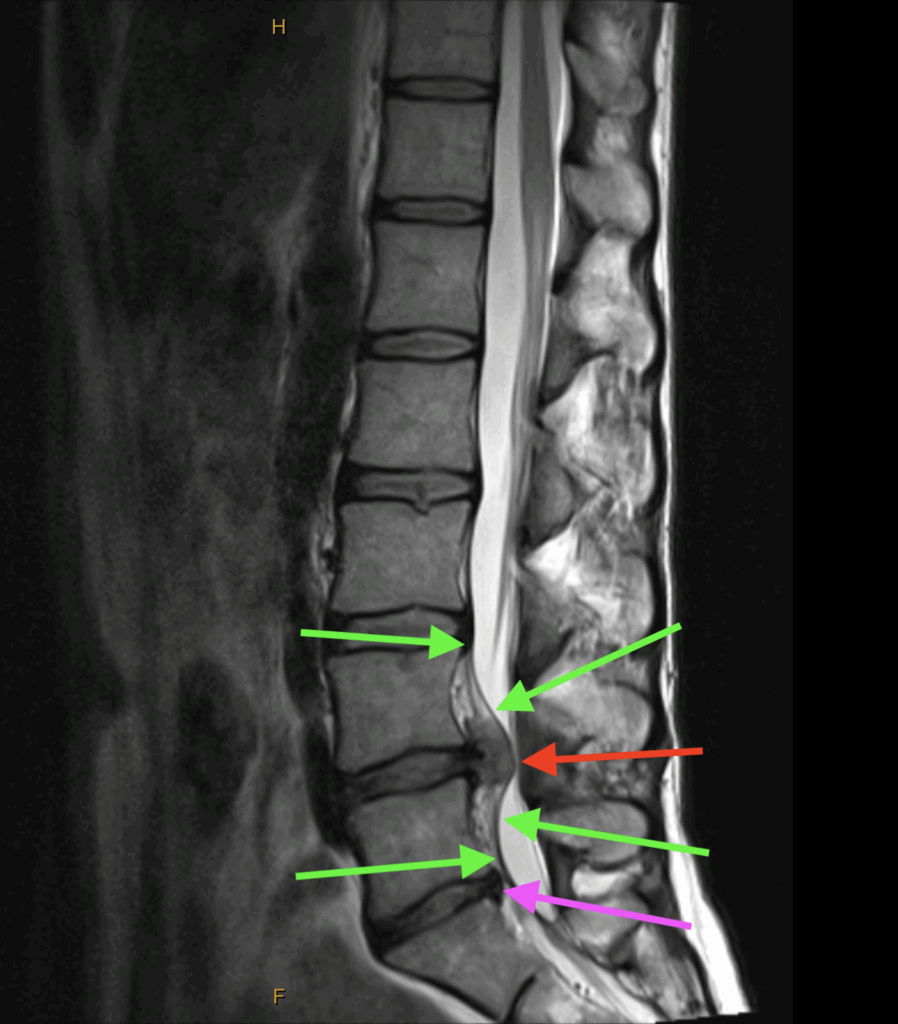
T2 Sagittal
The green arrows indicate the Posterior Longitudinal Ligament. Note how it’s been torn off the anterior wall of the central canal by the extruded disc material. The mottled appearance between the ligament and the anterior wall is blood and torn tissue.
The red arrow indicates the mass of extruded nuclear material.
The purple arrow indicates the desiccated remnants of the previous L5-S1 disc.
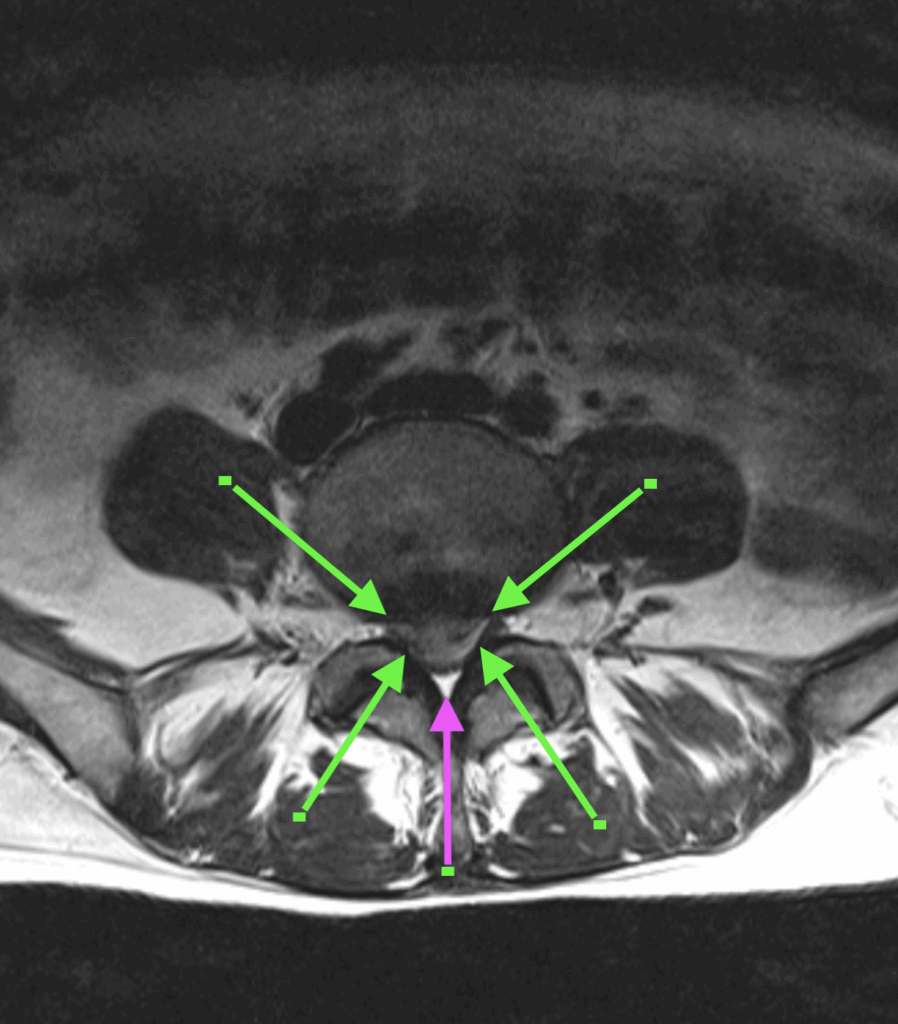
T2 Axial
The green arrows indicate the margins of the extruded disc material. Between the tips of each arrow we can see where the nerves of the Cauda Equina have been forced apart and into the lateral recess.
The purple arrow indicates the remaining space in the central canal.

There was no question that Joely needed spinal decompression surgery as soon as possible.
One the way home we called a local GP near where we lived and asked for the first available appointment. When we got there we told the GP what had happened and said that Joely needed a referral for a microdiscectomy, stronger pain relief and muscle relaxants.
The GP was very reluctant, so I showed him the MRI to which he responded “I can’t read those”. So I pointed out the disc injury.
He then said that “We don’t normally suggest surgery for back pain. We normally prescribe anti-inflammatories and six weeks of rest and Physiotherapy.” At this stage patience was running thin but I summoned all my calmness and said that without surgery she will mostly likely suffer permanent paralysis at best. He very reluctantly wrote the referral and gave Joely a prescription for Endone and Valium.
Not all GPs can read MRIs. They generally rely on the Radiologist’s report for all image interpretation. This approach cuts back on the time they need to spend learning to do it and then refining their skills. It also means that if something gets missed by the Radiologist they’re not liable. That’s fine until they’re confronted with a case like this.
This experience also highlights the failings of a formulaic approach to health care, whether it be Medicine, Chiropractic, Psychology or whatever. It’s much easier to have a reflex response to “back pain” than to make the effort to understand it’s complexities and then respond according to proper diagnostic procedures and clinical skill.
Had Joely been any other patient who’d presented with this injury and followed that advice, at best she would have ended up paraplegic and incontinent, at worst she would have died.
After she had the surgery she wrote to the GP to tell him what had happened. To his credit, he was very apologetic.
Monday
We had a very difficult night with only fleeting periods of sleep. By the morning Joely had started to develop foot drop.
The peripheralisation was on the move and starting to involve motor neurons.
We called our dear friend and Orthopædic Surgeon Dr David de la Harpe as soon as his rooms were open and asked for the first available appointment, which was at 9:00am on Tuesday.
Once again, the importance of inter-professional dialogue and cooperation cannot be understated.
I knew David from University. He started in Medicine at Melbourne, then transferred over to Chiropractic at what began as ICC-PIT but later became RMIT. He practiced for a couple years as a Chiropractor before returning to Medicine to finish his degree and then on to specialise in Orthopædics and Microdiscectomy. Last time we spoke about that topic he said that he was doing around 700 per year, when the average Neurosurgeon does around 20-30 per year. It would be difficult to overstate his expertise, knowledge and experience.
Tuesday
By the time we saw David he’d already seen the MRI images online. There was no need for any further examination. David said that he’d admit Joely to a ward immediately but he needed his “A-Team” to help him with this case, which would mean waiting until Thursday before the surgery could be performed.
The “A-Team” was Dr Tim Hurren, a Specialist Assistant Surgeon and Dr Nola Schenk Anesthetist.
He also explained that there was so much tension on the dura that there was a high risk of it splitting lengthwise if it was disturbed. He went on to say that when that happens the nerves of the Cauda Equina spill out into the canal like cooked spaghetti, the CSF runs out of the longitudinal split and patient dies on the table. That meant that he and his Assistant Surgeon had to coordinate both the timing and degree of their excisions so the dura was not pulled one way or the other as the tension was relieved.
Wednesday
Joely’s leg was now effectively flaccid, she had lost both the anterior and posterior tibial pulses and her lower leg was starting to change colour.
The nerves were in such stress now that they were shutting down completely, taking out the control of arterial wall muscle fibres. The limb was now in danger of dying.
Thursday
Joely was first on the list, and returned to the ward after two and a half hours of surgery.
The incision was about 25mm long. After opening up down to the posterior vertebral elements a small fenestrating laminectomy was performed on each side and the dura very carefully elevated. David and Tim then coordinated their excisions so they happened simultaneously, thereby reducing the risk of an asymmetric load causing a dural rupture. They removed all the extruded disc material, scraped out all nuclear remnants from inside the disc; suctioned and irrigated it before finally packing it with antibiotic pellets.
One could easily think that Knowledge Is Power in these circumstances, but it is definitely a two edged sword. The more you know, the more you know what can go wrong and the consequences.
I didn’t know if I’d get my wife back with a functional leg, normal bowel and bladder control, or at all. I was dreading the thought that the first person I’d see might be David with a concerned look on his face, rather than Joely on a gurney. That was one of the frightening two and half hours of my life.
David came into the room and told us that surgery was “extremely challenging but successful” and now it was up to Joely’s body to do the rest.
Joely spent the next three days in hospital with a drain in the wound and a steady supply of opioids and antibiotics.
After leaving hospital, Joely spent most of her days in bed with occasional very short walks. Initially only to the bathroom or around the house. By the 6 week mark she could walk around the yard provided she used walking poles. She still needed opioids.
It’s now seven years since the injury and she still has significant disability. Numbness extends down the back of her thigh to the knee, then again from the lower calf to the sole of her foot. She has a marked limp and struggles with uneven ground because she doesn’t know where her foot is or what’s under it. There is noticeable muscle wasting in her left calf.
What Are The Take Home Points?
- Understand Adjacent Joint/Segment Disease – If a patient has disc loss at one level, they’re at risk of a disc injury above.
- Each subsequent injury is usually worse than the previous.
- Never hesitate to get good quality imaging immediately.
- Learn to read and understand MRI.
- Develop and maintain close working relationships with other professionals.
- Rapidly peripheralising symptoms are an emergency.
- Permanent losses happen quickly.
The “Sarah/Joely” case was daunting but they’re not all like that.

